

CRISIS PROPORTIONS

Features
Audrey Fraizer
Opioid addiction and its consequences made Dan Snarr an outspoken critic of an epidemic keeping a stranglehold on the United States.
And it’s a position that’s neither enviable nor expected, considering the personal toll on his family and his religion. Snarr is a Mormon, which is relevant to his story. He is a high priest in the Church of Jesus Christ of Latter-day Saints (LDS), a faith that spurns the use of drugs and alcohol.
Snarr’s son Denver, also a devout member of the LDS church, was only 25 when he died from a prescription overdose in 2005. Doctors had prescribed painkillers following surgery for an injury caused while playing for the Murray High School rugby team, and the prescriptions continued for each subsequent injury the athletic Denver experienced in his young adult life.
“He kept getting hurt,” said Snarr, former mayor of Murray, Utah (USA), a suburb directly south of Salt Lake City. “After his third major surgery, he was hooked. He was doctor shopping.”
The Snarr family tried every avenue available to help Denver. They met with elders from their tight-knit LDS community. They went to family counseling. Denver voluntarily attended an addiction recovery program and was taking methadone to wean himself away from the drugs. They talked to him about the dangers and reassured him.
“We said repeatedly how much he was loved,” Snarr said. “We assured him that the addiction made him no less in our eyes.”
Denver died of a suspected overdose of methadone and sleeping pills hours after telling his father he was getting off the drugs. He died before help arrived and nearly a decade before naloxone—a medication that can reverse an opioid overdose—was accessible outside of EMS.
“There’s a chance he could have been saved,” Snarr said.
Instead, he died at the crux of an epidemic.
According to the Centers for Disease Control and Prevention (CDC) (2015):
- Heroin and prescription painkiller abuse, a class of drugs known as opioids, caused more than 50,000 deaths from drug overdoses in the U.S.
- Heroin deaths rose 23 percent in one year, to 12,989. Deaths from synthetic opioids, including illicit fentanyl, rose 73 percent to 9,580. And prescription painkillers took the highest toll.
- Abuse of drugs like Oxycontin and Vicodin killed 17,536, an increase of 4 percent.1
Utah ranks fourth highest per capita in the nation for drug overdose deaths, a problem state officials are addressing through legislation, safe drug disposal campaigns, and, recently, authorizing pharmacies to dispense naloxone without a prescription.
What is an opioid?
Opioids are a class of drug used to reduce pain. Prescription opioids are used to treat moderate to severe pain. Common types are oxycodone (OxyContin), hydrocodone (such as Lortab and Vicodin), morphine, and methadone. Fentanyl is a synthetic opioid pain reliever. It is many times more powerful than other opioids and is approved for treating severe pain. Heroin is an illegal opioid. From 1999 to 2013, the amount of opioids dispensed in the U.S. nearly quadrupled.
Oxycodone is a semi-synthetic opiate developed in 1916 as an effort to find non-addictive alternatives to narcotic drugs (morphine and heroin), which were commonly used in medicine before and during World War I. Like all opiates, oxycodone works by binding to opioid receptors in the brain and spinal cord for relieving pain and, at higher doses, for a euphoric effect.
In the past, oxycodone and other opiate drugs were prescribed sparingly and mainly for short-term pain. However, changes to government recommendations and aggressive marketing by pharmaceutical companies led to a dramatic increase in the last 25 years in prescriptions of oxycodone for long-term use in patients with chronic pain.3
Preventive and lifesaving strategies
Naloxone
Naloxone is an antagonistic medication that saves lives by counteracting the effects of opioid overdose. First cited in 1961, It was not the first and only medication to counteract the effects of an opioid overdose, but it was considered a medical breakthrough in reversing respiratory depression common in overdoses of synthetic and natural opioid related substances.4 In 1971, the Food and Drug Administration (FDA) licensed naloxone for opiate overdoses by intravenous or intramuscular injection, stating that access to the medication would require a prescription from an authorized health care provider. The FDA approved an intranasal naloxone applicator in November 2015.
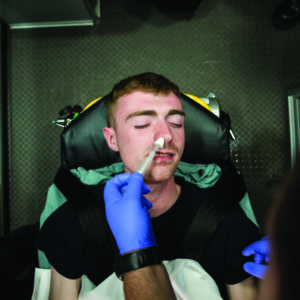
A study involving systematic review of overdose prevention programs (OOPPS) that include the distribution of naloxone clearly supports the drug’s effectiveness:
Naloxone was used successfully by participants in all but one reviewed study, for a total of 1,949 reported naloxone administrations across 18 programs. Eleven studies reported 100% survival rate post–naloxone administration; the remaining articles reported a range of 83% to 96% survival.5
Paramedics arriving on scene can administer naloxone or, in the better-case scenario, someone on scene can administer it. The study cited also provided evidence suggesting that bystanders (mostly opioid users) can and will use naloxone to reverse opioid overdoses when properly trained.6
The Medical Priority Dispatch System™ (MPDS®) v13.0 established Post-Dispatch Instructions (PDIs) in Protocol 23: Overdose/Poisoning for both intramuscular and intranasal delivery of naloxone. The EMD provides the PDIs when the initial request is to help the caller administer naloxone and in situations in which the patient’s condition worsens during the call (becomes not alert or unconscious).
Callers in the Boston, Massachusetts (USA), area may soon have easier access to naloxone when reporting a drug overdose to 911 through an online PSAP registry of publicly available naloxone for bystander administration.
Dr. Scott Goldberg, EMS Director in the Emergency Department at Brigham and Women's Hospital in Boston, likened the program to community AED access. In case of a sudden cardiac arrest, dispatchers at many 911 centers throughout the country can locate the closest publicly available AED through an online registry and provide that information to the caller while at the same time dispatching EMS and providing bystander CPR instructions.
Naloxone access would work the same way. A call comes into the center, the dispatcher gathers information, and, in the case of a drug overdose, the dispatcher can pull up a registry to direct the caller to the closest possible naloxone emergency box. At the same time, a dispatcher using the MPDS can provide PAIs for administering the medication and send EMS response.

Goldberg said the proposal comes in response to the growing opioid crisis.
“The number of overdoses keeps climbing, and the severity is increasing as the drugs get stronger,” Goldberg said. “In a heroin overdose, we have minutes to reverse the effects. For fentanyl, it’s a matter of seconds.”
While logistics are in the planning, Goldberg said surveillance can provide statistics for optimal public access, such as in areas showing the highest density of overdose calls to 911 and EMS data on emergency overdose response.
Faster access to naloxone doesn’t solve the drug problem, Goldberg said. But it’s one of several measures to curb the alarming increase in death rates associated with opioid overdose.
“Drug addiction is a disease,” Goldberg said. “We’re trying to get naloxone in the hands of someone who can help as fast as possible in an overdose situation.”
Massachusetts is also one of more than two dozen states with a Prescription Drug Monitoring Program (PDMP). PDMPs provide clinicians with scheduled medication histories, helping identify patients that may be abusing medications. PDMPs also identify “doctor shopping” through reporting systems and surveillance to identify irresponsible prescribing.
PDMPs are another tool to fight the epidemic, Goldberg said.
“We’re increasing resources,” he said. “We’re increasing public awareness. This is not an easy problem to be solved, but hopefully things will get better through multiple approaches.”
Surveillance
Surveillance and multi-agency cooperation using and sharing CAD and electronic patient care reporting (ePCR) data is a strategy with the persistence to escalate the war against opioid abuse. Among other benefits, such as allowing clinical distinction at the onset of a 911 call to quickly identify an opioid overdose, the strategy can prevent abuse through detecting points of sale for law enforcement and encouraging individuals to seek treatment in the recovery from opioid dependency.
FirstWatch, a data gathering company headquartered in Encinitas, California (USA), was established in 1998, almost quite accidentally, when Todd Stout devised an algorithm to collect information for the EMS System in Kansas City, Missouri (USA) (then MAST). The company, independent of the ambulance service, now provides its expertise to more than 350 clients in North America.
FirstWatch monitors data in real time and replaces the tedious and often inaccurate process of manually reviewing all records in relation to an incident or situation. Clients choose the parameters and FirstWatch models the solution from best practice experience and asking what might be different for the specific client. Triggers are defined to draw the raw data from sources, including ProQA® and electronic Patient Care Records (ePCR), and the data is analyzed to complement pieces of the query.
The process is dynamic, said Stout, a former MAST Paramedic.
“Data gives us patterns,” he said. “It can create a picture of what’s going on at the local level. It tells us where things are happening.”
The real-time gathering and surveillance make FirstWatch an ideal tool in the battle to prevent opioid use and abuse, from the point of sale to helping an overdose patient. The data also focuses efforts of law enforcement, social workers, and others relevant to the issue.
“FirstWatch can adapt surveillance to the community,” Stout said. “We also take away the burden of gathering data so that the agency can concentrate on what needs to be done.”
ProEMS, in Cambridge, Massachusetts, and Richmond Ambulance Authority (RAA), Richmond, Virginia (USA), are among agencies using FirstWatch algorithms in the communication center and the field to detect opioid overdoses and share that information with local agencies that can intervene in real time.
RAA partners with the Richmond Police Department Narcotics Task Force to confirm an Emergency Dispatcher’s interpretation of a call in the communication center with those actually occurring in the field.
“It allows us to look at the point of OD, which we know, versus the suspected point of sale,” said Rob Lawrence, RAA Chief Operating Officer. “They usually have some intelligence, but more often than not, sale and consumption are not far apart.”
RAAuses FirstWatch to identify clusters of real-time activity and syndromic activity. From the data, RAA can calculate total numbers of potential opioid overdoses from clinical records in periods of high activity and monitor the number of naloxone doses administered per patient.
“We are seeing the more complex the mix, the more naloxone needed,” Lawrence said. “At this point [due to lab backup] we have no definitive indication of what is in the heroin mix, but what we have seen after the fact is that more fentanyl, the more naloxone required.”
They also flag patients who refuse transport to encourage medical attention, at some point, and recovery.
“We work hard to get them help,” Lawrence said.
Good data is everything, according to Bill Mergendahl, Chief Executive Officer, ProEMS. Data FirstWatch pulls from multiple sources gives an in-depth view of their system, and the data can be segregated to support different outcomes. Triggers to collect data specific to opioid use depend on a list of customized symptomatic chief complaints taken from a caller’s narrative.
Real-time information geocoded to the caller’s location initiates response. ProEMS shares clinical overdose data with Cambridge Public Health Department and tracks calls according to positive response related to naloxone administration.
Tracking has multiple benefits. It can target higher users of emergency services and signal a potential medical situation based on patient history. Data can hasten intervention.
In an opioid emergency, ProEMS can provide paramedics trained as recovery coaches. The coaches can provide the patient with contact information and referral.
“Like everyone in EMS, we are frustrated by the revolving door,” Mergendahl said. “We have the resources to make an impact and help patients who are trying to recover.”
The system’s not failproof, Mergendahl said. For example, EMS personnel cannot identify every overdose, nor can they save every patient experiencing an overdose. But it’s a start that brings with it the opportunity to exchange information and strategize.
“We learn from collaboration,” Mergendahl said.
Legislation
State and federal regulations affect the delivery of patient care and the availability of treatment options.
The Federal Comprehensive Addiction and Recovery Act (CARA), signed in July 2016, includes provisions to update best practices for pain management and pain medications, study the prevalence of neonatal abstinence syndrome, authorize funds for expanded treatment, and train law enforcement officers and first responders in the use of naloxone.

The CDC awarded $12.8 million in grants to 12 states to better track opioid involved overdoses over a three-year-period starting in fall 2016. States will use the program funds to increase the timeliness of reporting nonfatal and fatal opioid overdoses and share their data to improve multi-state surveillance and response.7
The grant was in addition to $18 million Congress appropriated to the CDC for funding the Prescription Drug Overdose: Data-Driven Prevention Initiative. The three-year grants were awarded to 13 states and the District of Columbia and targets development of a web query system that provides data on prominent risk factors for opioid overdoses and drug overdose mortality data across the U.S. This data dashboard will also help track the progress of U.S. states implementing prevention programs and policies versus those that are not.8
According to recent figures, 37 states and the District of Columbia had enacted some form of a Good Samaritan or 911 drug immunity law. In general, these laws provide immunity from supervision violations, low-level drug possession, and use offenses when calling 911 for assistance when experiencing an opiate-related overdose, as either a bystander or the individual taking the drug.9
Turning pain into action
Snarr turned the pain of Denver’s death into action. He is a community volunteer, regularly finding what needs to be done, particularly by the elderly, such as replacing water heaters, shoveling snow from driveways, or running errands. He is an “ear” for LDS families experiencing drug abuse problems within their homes, and he is an outspoken advocate of discussing the drug problem to promote legislation and prevention.
“I talk to people all the time,” Snarr said. “They don’t know what to do. We have to get to the root. Unless we do, we will never know how to address the problem effectively.”
No matter the basis of addiction, Snarr grows impatient waiting for someone or something to get to the bottom of the problem and work up from there.
“It’s not only about me and my son,” he said. “It’s about these young people and adults who could be in the same situation trying to cope with pain and suffering. It saddens me.”
Sources
1 Stobbe M. “Record 50,000 U.S. Drug Overdose Deaths in 2015.” Associated Press. 2016; Dec. 13. http://www.allgov.com/news/controversies/record-50000-us-drug-overdose-deaths-in-2015-161213?news=859907 (accessed Dec. 13, 2016).
2 “Injury Prevention & Control: Opioid Overdose.” Centers for Disease Control and Prevention. 2016; March 14. https://www.cdc.gov/drugoverdose/opioids/index.html (accessed Dec. 12, 2016).
3 MacLaren E. “Oxycodone History and Statistics.” DrugAbuse.com. http://drugabuse.com/library/oxycodone-history-and-statistics/ (accessed Dec. 13, 2016).
4 “A Brief Timeline of Naloxone for Reference.” Future Moves. 2015; Jan. 7. https://futuremoves.wordpress.com/2015/01/07/a-brief-timeline-of-naloxone-for-reference/
(accessed Dec. 12, 2016).
5 Clark A, Wilder C, Winstanley E. “A Systematic Review of Community Opioid Overdose Prevention and Naloxone Distribution Programs.” American Society of Addiction Medicine. 2013; Volume 8 (No. 3. 2014: May/June), 153-163.
6 See note 5.
7 “Enhanced State Surveillance of Opioid Involved Morbidity and Mortality.” 2016; Oct. 20. https://www.cdc.gov/drugoverdose/foa/state-opioid-mm.html (accessed Dec. 12, 2016).
8 “Data-Driven Prevention Initiative.” Centers for Disease Control and Prevention. 2016; Oct. 20. https://www.cdc.gov/drugoverdose/foa/ddpi.html (accessed Dec. 12, 2016).
9 “Drug Overdose Immunity and Good Samaritan Laws.” National Conference of State Legislatures. 2016. http://www.ncsl.org/research/civil-and-criminal-justice/drug-overdose-immunity-good-samaritan-laws.aspx#Calling%20911 (accessed Dec. 13, 2016).




